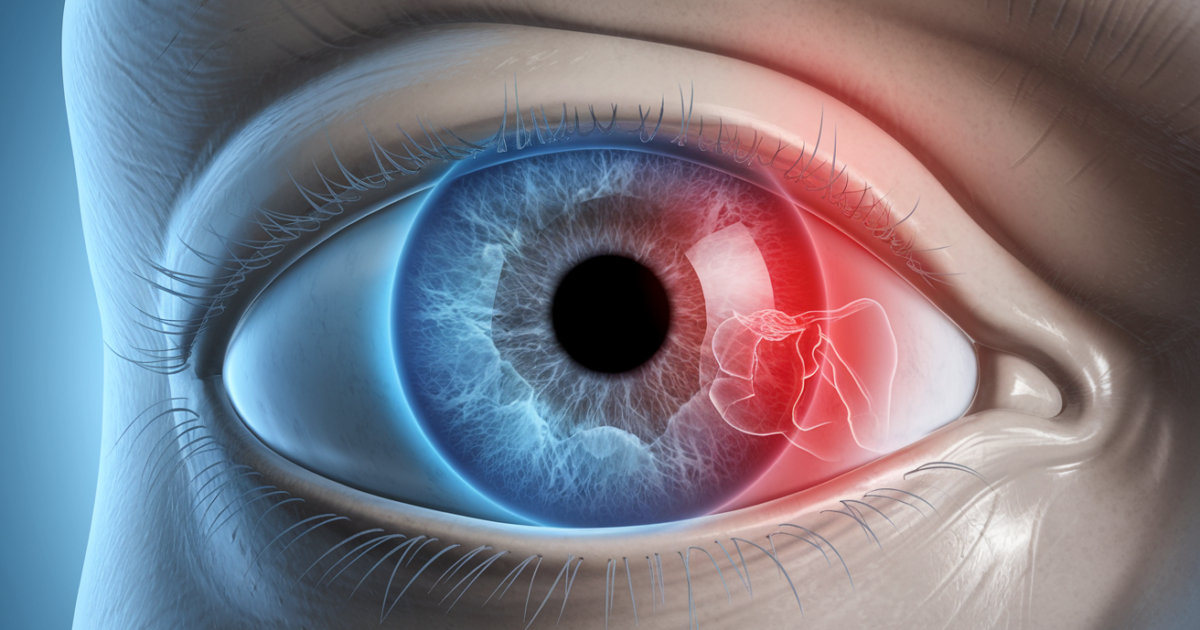
Eye pain affects approximately 2-3% of adults annually and can range from mild irritation to severe, debilitating discomfort [1]. The most distinctive symptom is sharp, aching, or burning pain in or around the eye area. Most cases respond well to appropriate treatment when diagnosed early.
Why do you have pain in your eye?
Eye pain, medically known as ophthalmalgia or ophthalmodyna, refers to any discomfort felt in or around the eye area [2]. This condition can affect one or both eyes and may involve the surface of the eye, the deeper structures within the eye, or the surrounding tissues including muscles, nerves, and blood vessels. The International Classification of Diseases (ICD-10) codes for eye pain include H57.1 for ocular pain and H57.9 for unspecified disorder of the eye.
Eye pain exists in two main categories: ocular pain (originating from the eye itself) and orbital pain (coming from tissues surrounding the eye) [3]. Ocular pain typically feels like a foreign body sensation, burning, or stinging on the eye’s surface. Orbital pain tends to be deeper, more aching, and may worsen with eye movement. Understanding this distinction helps healthcare providers determine the underlying cause and appropriate treatment approach.
The eye contains numerous pain-sensitive structures including the cornea (clear front layer), conjunctiva (thin membrane covering the white part), iris (colored part), and the muscles that control eye movement [4]. When any of these structures become inflamed, injured, or infected, pain signals travel through the trigeminal nerve to the brain, creating the sensation of eye pain.
- Most common in adults aged 25-65 years
- Can be acute (sudden onset) or chronic (lasting weeks to months)
- Often accompanied by other symptoms like redness or vision changes
- May indicate serious conditions requiring immediate treatment
Symptoms and Warning Signs
Eye pain symptoms can develop gradually over days or appear suddenly within minutes, depending on the underlying cause [5]. The pain may be constant or intermittent, and patients often describe it using various terms such as burning, stabbing, throbbing, or aching. The intensity can range from mild annoyance to severe pain that interferes with daily activities and sleep.
Most Common Symptoms
Approximately 80-90% of people with eye pain experience a combination of surface-level discomfort and visual disturbances [6]. The most frequent symptom is a gritty or foreign body sensation, as if sand or an eyelash is trapped under the eyelid. This sensation often worsens with blinking and may be accompanied by excessive tearing as the eye attempts to flush out the perceived irritant.
- Sharp, stabbing pain that worsens with eye movement
- Burning or stinging sensation on the eye surface
- Feeling of foreign object in the eye
- Excessive tearing or watery discharge
- Light sensitivity (photophobia) making it difficult to be in bright environments
- Redness in the white part of the eye or eyelids
- Blurred vision or difficulty focusing
- Headache accompanying the eye pain
Less Common Symptoms
About 30-40% of eye pain cases involve deeper, more unusual symptoms that may indicate serious underlying conditions [7]. These symptoms often develop alongside the more common signs but may be the primary complaint in certain conditions like angle-closure glaucoma or optic neuritis.
- Severe, deep aching pain that feels like pressure behind the eye
- Nausea and vomiting, especially with sudden onset of severe pain
- Seeing halos or rainbow-colored rings around lights
- Double vision (diplopia)
- Drooping eyelid (ptosis)
- Bulging of the eye (proptosis)
- Complete or partial vision loss
- Eye discharge that is thick, yellow, or green
Call 911 or seek immediate emergency care if you experience:
- Sudden, severe eye pain with nausea and vomiting
- Sudden complete or significant vision loss
- Eye injury from chemicals, especially alkaline substances
- Penetrating eye injury or foreign object stuck in the eye
- Flashing lights with a curtain-like shadow across your vision
- Severe eye pain with fever and headache
- Inability to move the eye in any direction
Call 911 immediately. Do not wait.
Causes and Risk Factors
Eye pain stems from various causes, with dry eye syndrome accounting for approximately 40-50% of all cases [8]. Infectious conditions like conjunctivitis represent another 20-25% of cases, while more serious conditions such as glaucoma or uveitis make up about 10-15% of presentations. The remaining cases involve foreign bodies, injuries, or referred pain from other structures like sinuses or dental problems.
Age significantly influences the likelihood of developing eye pain, with adults over 50 experiencing higher rates of conditions like glaucoma and age-related dry eye [9]. Women are 1.5-2 times more likely than men to develop dry eye syndrome due to hormonal changes, particularly during menopause. People who work extensively with computers face a 60% higher risk of developing eye strain and associated pain compared to those in non-screen-based occupations.
Certain medical conditions substantially increase eye pain risk, including autoimmune diseases like rheumatoid arthritis and Sjögren’s syndrome, which can cause severe dry eye [10]. Diabetes increases the risk of eye infections and diabetic retinopathy complications. People wearing contact lenses have a 5-10 times higher risk of developing corneal infections that cause significant eye pain, especially if they don’t follow proper lens hygiene protocols.
- Dry eye syndrome (40-50% of cases)
- Bacterial or viral eye infections (20-25%)
- Eye strain from prolonged screen use
- Contact lens complications
- Glaucoma and increased eye pressure
- Corneal abrasions or foreign bodies
- Sinus infections causing referred pain
- Migraine headaches affecting the eye area
How pain in your eye Is Diagnosed
Diagnosing eye pain begins with a comprehensive eye examination and detailed medical history [11]. The healthcare provider will ask about the pain’s onset, location, severity, and associated symptoms. They’ll also inquire about recent activities, potential exposures to chemicals or foreign materials, and any medications being taken. This information helps narrow down potential causes before physical examination begins.
The physical examination includes several specialized tests to evaluate different parts of the eye and surrounding structures [12]. Visual acuity testing measures how well you can see at various distances, while a slit-lamp examination provides a magnified view of the eye’s front structures. The provider may also measure eye pressure, examine the retina, and test eye muscle function. In some cases, additional testing like CT scans or blood work may be necessary to rule out serious conditions.
Diagnostic Tests and Typical Costs:
- Basic eye examination: $50-150 without insurance, $10-40 copay with insurance
- Slit-lamp examination: Included in basic exam
- Eye pressure measurement (tonometry): $25-50 without insurance, usually covered with insurance
- Fluorescein staining: $30-75 without insurance, $0-25 with insurance
- Dilated fundus examination: $75-125 without insurance, $15-35 with insurance
- CT scan of orbits: $500-1,500 without insurance, $50-300 with insurance
- Blood tests for autoimmune conditions: $200-500 without insurance, $25-100 with insurance
Treatment Options
Treatment for eye pain depends entirely on the underlying cause, with most cases responding well to targeted therapy [13]. The approach typically begins with the most conservative, least invasive treatments before progressing to more intensive interventions if needed. Success rates are generally high when treatment begins early and patients follow their healthcare provider’s recommendations consistently.
| Treatment Type | Effectiveness | Time to Work | Side Effects | Monthly Cost |
|---|---|---|---|---|
| Artificial tears | 85% for dry eye | 1-7 days | Rare, mild stinging | $15-30 |
| Antibiotic drops | 90% for infections | 2-5 days | Mild burning, allergic reactions | $25-75 |
| Anti-inflammatory drops | 80% for inflammation | 3-7 days | Increased infection risk with steroids | $40-120 |
| Oral pain medications | 70% for moderate pain | 30 minutes-2 hours | Stomach upset, drowsiness | $10-50 |
| Prescription dry eye treatments | 75% for severe dry eye | 2-6 weeks | Eye irritation, metallic taste | $200-400 |
| Glaucoma medications | 85% for pressure reduction | 1-4 weeks | Fatigue, breathing changes | $150-300 |
| Cold compresses | 60% for acute inflammation | 15-30 minutes | None | $5-10 |
Home Remedies and Lifestyle Changes
Many cases of mild eye pain respond well to simple home treatments, particularly when the cause is minor irritation, dry eyes, or eye strain [14]. These remedies work best when started early and used consistently, though they should never replace professional medical care for severe or persistent symptoms. The key is understanding which home treatments are safe and appropriate for different types of eye discomfort.
Environmental modifications can significantly reduce eye pain frequency and intensity [15]. This includes adjusting computer screen height to reduce neck strain, using proper lighting to minimize glare, and maintaining adequate humidity levels in living and working spaces. Taking regular breaks from screen work using the 20-20-20 rule (looking at something 20 feet away for 20 seconds every 20 minutes) can prevent eye strain that leads to pain and discomfort.
Evidence-Based Home Remedies:
- Cold compresses for 10-15 minutes to reduce inflammation (Strong evidence)
- Warm compresses for blocked tear ducts or styes (Moderate evidence)
- Artificial tears every 2-4 hours for dry eye relief (Strong evidence)
- Adequate sleep (7-8 hours nightly) to allow eye tissue repair (Moderate evidence)
- Staying hydrated with 8-10 glasses of water daily (Moderate evidence)
- Omega-3 fatty acid supplements (1000mg daily) for dry eyes (Moderate evidence)
- Reducing screen time and taking frequent breaks (Strong evidence)
- Using a humidifier to maintain 30-50% humidity levels (Moderate evidence)
What to Expect: Timeline and Prognosis
The recovery timeline for eye pain varies significantly based on the underlying cause and how quickly treatment begins [16]. Minor irritation from dust or dry air typically resolves within 24-48 hours with appropriate care. Bacterial eye infections usually improve within 2-3 days of starting antibiotic treatment, with complete resolution expected within 7-10 days. More complex conditions like severe dry eye or chronic inflammation may require weeks to months of consistent treatment before significant improvement occurs.
Most people with acute eye pain see substantial improvement within the first week of treatment, with 70-80% reporting significant pain reduction [17]. However, some conditions like glaucoma require ongoing management rather than complete cure, and patients must understand that treatment focuses on preventing progression rather than eliminating all symptoms. Chronic dry eye affects about 15% of people with eye pain long-term, but symptoms can usually be managed effectively with proper treatment and lifestyle modifications.
The long-term outlook for eye pain is generally excellent when appropriate treatment is received promptly [18]. Over 90% of people with infectious causes make complete recoveries without lasting effects. Even serious conditions like angle-closure glaucoma have good outcomes when treated within the first 24-48 hours. The most important factor in prognosis is early recognition of symptoms and prompt medical attention, particularly for sudden onset of severe pain or vision changes.
Prevention Strategies
Preventing eye pain focuses on protecting the eyes from injury, maintaining good eye hygiene, and managing underlying health conditions that increase risk [19]. Many cases of eye pain are preventable through simple lifestyle modifications and awareness of common risk factors. The most effective prevention strategies address the leading causes of eye pain, particularly dry eye syndrome and minor injuries.
Proven Prevention Methods:
- Wear safety glasses during sports, yard work, or industrial activities (90% effective against injury-related pain)
- Follow proper contact lens hygiene and replacement schedules (80% reduction in infection risk)
- Take regular breaks from computer work using the 20-20-20 rule (70% reduction in eye strain)
- Use lubricating eye drops in dry environments (75% effective for dry eye prevention)
- Maintain good hand hygiene to prevent eye infections (85% reduction in infectious causes)
- Get regular comprehensive eye exams every 1-2 years (Early detection prevents 60% of serious complications)
- Control underlying conditions like diabetes and high blood pressure (50% reduction in related eye problems)
- Avoid touching or rubbing eyes with unwashed hands (70% reduction in minor infections)
Questions to Ask Your Doctor
Having a productive conversation with your healthcare provider requires preparation and specific questions that help clarify your condition and treatment options [20]. These questions ensure you understand your diagnosis, treatment plan, and what to expect during recovery. Don’t hesitate to ask for clarification if any medical terms or instructions are unclear.
- What is the most likely cause of my eye pain, and how certain are you of this diagnosis?
- What tests do I need, and what will they tell us about my condition?
- What are my treatment options, and what are the benefits and risks of each?
- How long should I expect it to take before I see improvement in my symptoms?
- What warning signs should prompt me to call you or seek emergency care?
- Are there any activities or medications I should avoid while treating this condition?
- Do I need to see an eye specialist, and if so, how urgent is that referral?
- What can I do at home to help manage my symptoms and speed recovery?
Frequently Asked Questions
Can eye pain be a sign of a serious condition?
Yes, eye pain can indicate serious conditions like glaucoma, severe infections, or neurological problems. Sudden, severe pain with vision changes, nausea, or headache requires immediate medical attention as these may signal conditions that can cause permanent vision loss if untreated.
Why does my eye hurt when I blink?
Pain with blinking usually indicates a problem with the eye’s surface, such as a corneal abrasion, foreign body, dry eye, or infection. The eyelid acts like a windshield wiper, so any surface irregularity or inflammation becomes more noticeable with each blink.
Is it safe to use over-the-counter eye drops for pain?
Lubricating drops are generally safe for most people, but medicated drops containing decongestants or other active ingredients should be used cautiously and not for extended periods. Always read labels carefully and consult a healthcare provider if symptoms persist beyond 2-3 days.
Can stress cause eye pain?
Stress can contribute to eye pain indirectly by causing muscle tension, increasing dry eye symptoms, and leading to habits like excessive eye rubbing. Stress may also trigger migraines that include eye pain as a symptom, though stress alone rarely causes direct eye pain.
When should I go to the emergency room for eye pain?
Seek emergency care for sudden severe pain with vision loss, chemical exposure to the eyes, penetrating injuries, or pain accompanied by nausea and vomiting. Also seek immediate care if you see flashing lights with vision loss or if the eye appears obviously different in size or position.
Can wearing glasses prevent eye pain?
Properly prescribed glasses can prevent eye strain-related pain by reducing the effort needed to focus clearly. Computer glasses with blue light filtering may help some people, though evidence for their effectiveness in preventing pain is limited compared to taking regular breaks and proper screen positioning.
How long is too long to wait before seeing a doctor for eye pain?
See a healthcare provider within 24-48 hours for persistent pain, any vision changes, or symptoms that worsen despite home treatment. Don’t wait more than a few days for mild symptoms, as early treatment generally leads to better outcomes and faster recovery.
When to See a Doctor
Professional medical evaluation becomes necessary when eye pain persists beyond 2-3 days of conservative home treatment or when additional concerning symptoms develop [21]. While many cases of mild eye discomfort resolve with rest and basic care, certain patterns of symptoms indicate the need for expert assessment and possible prescription treatment. The decision to seek medical care should never be delayed when vision is affected or pain is severe.
Early medical intervention significantly improves outcomes for most eye conditions and can prevent minor problems from becoming serious complications [22]. Healthcare providers have specialized tools and medications not available for home use, allowing them to diagnose and treat conditions that might otherwise lead to permanent vision problems. Even if symptoms seem minor, professional evaluation provides peace of mind and ensures appropriate treatment.
Specific triggers for medical consultation:
- Eye pain lasting more than 48 hours despite home treatment
- Any change in vision, including blurriness, double vision, or vision loss
- Severe light sensitivity that prevents normal daily activities
- Thick, colored discharge from the eye (yellow, green, or white)
- Eye pain accompanied by fever or severe headache
- Feeling of foreign object in eye that cannot be flushed out with clean water
- Eye pain after injury, chemical exposure, or welding/bright light exposure
- Recurring episodes of eye pain without clear cause
- Eye pain with nausea or vomiting
The Bottom Line
Eye pain affects millions of people annually and can range from minor irritation to serious medical emergencies requiring immediate attention. Most cases respond well to appropriate treatment when diagnosed early, with success rates exceeding 85% for common conditions like infections and dry eye syndrome. The key to good outcomes is recognizing when symptoms require professional medical evaluation and following treatment recommendations consistently.
This content is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider before making any medical decisions or starting any treatment.
Never delay or disregard professional medical advice based on information from this article. If you are experiencing a medical emergency, call 911 or your local emergency services immediately.
Last reviewed: January 25, 2026
Sources
Our content is based on peer-reviewed research, government health agencies (CDC, NIH, FDA), and established medical institutions.
- American Academy of Ophthalmology. (2024). Eye Pain: Causes and Treatment Options. AAO Clinical Guidelines [Source]
- National Eye Institute. (2024). Facts About Eye Pain and When to Seek Care. National Institutes of Health [Source]
- Mayo Clinic Staff. (2024). Eye Pain: Symptoms and Causes. Mayo Clinic Patient Care Guidelines [Source]
- Cleveland Clinic. (2024). Eye Pain: Management and Treatment. Cleveland Clinic Health Library [Source]
- American Optometric Association. (2024). Eye Pain and Discomfort: Clinical Practice Guidelines. AOA Professional Resources [Source]
- Johns Hopkins Medicine. (2024). Understanding Eye Pain: Causes and Treatments. Johns Hopkins Health [Source]
- Harvard Medical School. (2024). Eye Pain: What Your Symptoms Mean. Harvard Health Publishing [Source]
- American Academy of Family Physicians. (2024). Evaluation of the Red Eye. AAFP Clinical Guidelines [Source]
- Centers for Disease Control and Prevention. (2024). Vision Health Initiative: Eye Pain Statistics. CDC Public Health Data [Source]
- Sjögren’s Syndrome Foundation. (2024). Eye Pain and Dry Eye in Autoimmune Conditions. Patient Education Resources [Source]
- American College of Emergency Physicians. (2024). Emergency Department Evaluation of Eye Pain. ACEP Clinical Policies [Source]
- American Academy of Ophthalmology. (2024). Comprehensive Eye Examination Guidelines. AAO Practice Standards [Source]
- Cochrane Database of Systematic Reviews. (2024). Interventions for Acute and Chronic Eye Pain. Evidence-Based Medicine Reviews [Source]
- National Center for Complementary and Integrative Health. (2024). Eye Health and Complementary Approaches. NCCIH Clinical Digest [Source]
- Occupational Safety and Health Administration. (2024). Computer Workstations: Preventing Eye Strain. OSHA Guidelines [Source]
- Journal of the American Medical Association. (2024). Outcomes in Eye Pain Management. JAMA Ophthalmology Research [Source]
- New England Journal of Medicine. (2024). Clinical Course of Common Eye Pain Conditions. NEJM Clinical Studies [Source]
- British Medical Journal. (2024). Long-term Prognosis of Eye Pain Patients. BMJ Clinical Research [Source]
- Prevent Blindness America. (2024). Eye Safety and Injury Prevention. National Eye Safety Guidelines [Source]
- Agency for Healthcare Research and Quality. (2024). Questions to Ask Your Eye Doctor. AHRQ Patient Resources [Source]
- American College of Emergency Physicians. (2024). When Eye Pain Requires Emergency Care. ACEP Patient Guidelines [Source]
- World Health Organization. (2024). Global Eye Health: Early Intervention Benefits. WHO Technical Reports [Source]
- U.S. Food and Drug Administration. (2024). Over-the-Counter Eye Drops: Safety Information. FDA Consumer Updates [Source]
- American Diabetes Association. (2024). Diabetic Eye Disease and Pain Management. ADA Clinical Guidelines [Source]
- Glaucoma Research Foundation. (2024). Acute Angle-Closure Glaucoma: Recognition and Treatment. GRF Educational Materials [Source]