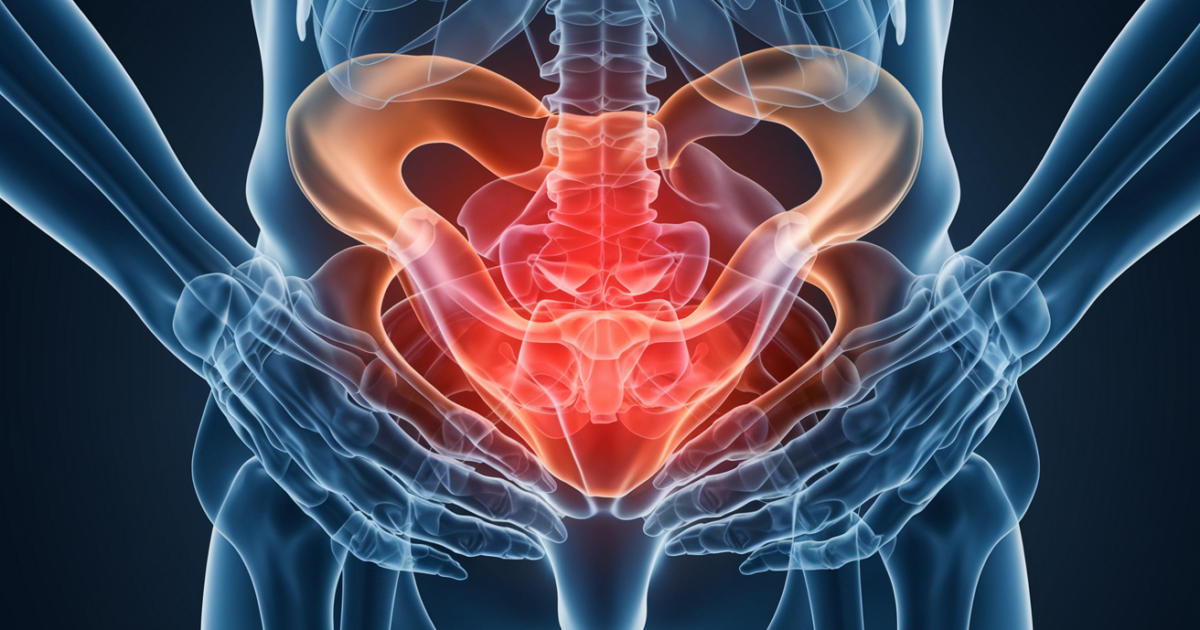
Pelvic pain during pregnancy is discomfort in the lower abdomen, groin, or back that affects up to 80% of pregnant women. The most distinctive symptom is sharp, shooting pain when walking or changing positions. Most cases respond well to physical therapy and supportive measures.
What is Pelvic pain in pregnancy?
Pelvic pain during pregnancy refers to discomfort experienced in the pelvic region, which includes the area between the hip bones, lower back, and upper thighs. This pain can range from mild discomfort to severe, debilitating symptoms that interfere with daily activities. The condition is medically classified under ICD-10 code O26.89 (Other specified pregnancy-related conditions) when it becomes clinically significant [1].
The pain occurs due to the complex changes happening in a woman’s body during pregnancy. Hormones like relaxin and progesterone soften ligaments and joints to prepare for childbirth, but this process can create instability and pain in the pelvic area. The growing baby also adds pressure to the pelvic structures, contributing to discomfort [2].
Healthcare providers often distinguish between different types of pregnancy-related pelvic pain, including symphysis pubis dysfunction (SPD), sacroiliac joint pain, and general pelvic girdle pain. Each type has slightly different characteristics but shares the common feature of affecting mobility and comfort during pregnancy [3].
- Most common during the second and third trimesters
- Can affect one or both sides of the pelvis
- Often worsens with activity and improves with rest
- Usually temporary, resolving after delivery
Symptoms and Warning Signs
Pelvic pain symptoms during pregnancy typically develop gradually, starting as mild discomfort and potentially progressing to more intense pain. The symptoms often fluctuate throughout the day, with many women reporting worse pain in the evening or after periods of activity.
Most Common Symptoms
Between 70-85% of women with pregnancy-related pelvic pain experience a characteristic pattern of symptoms that worsen with movement and improve with rest. The pain often feels like a deep ache or sharp, stabbing sensation that can make simple activities challenging. Walking, climbing stairs, and getting in and out of bed become particularly difficult as the pregnancy progresses [4].
- Sharp, shooting pain in the groin area when walking or turning over in bed
- Aching sensation in the lower back, especially after standing for long periods
- Clicking or grinding sounds from the pelvic joints when moving
- Difficulty separating legs, such as when getting out of a car
- Pain that radiates down the inner thighs or buttocks
- Worsening discomfort after physical activity or at the end of the day
- Stiffness in the pelvic area, particularly in the morning
Less Common Symptoms
Approximately 30-40% of women with pelvic pain during pregnancy may experience additional symptoms that can be more concerning or unusual. These symptoms might indicate a more severe case or a different underlying condition that requires medical attention [5].
- Numbness or tingling in the legs or pelvic area
- Severe pain that prevents walking or normal movement
- Bladder or bowel dysfunction accompanying the pelvic pain
- Swelling or visible changes in the pelvic area
- Pain that doesn’t improve with rest or position changes
Call 911 or seek immediate medical attention if you experience:
- Severe pelvic pain with heavy bleeding
- Signs of preterm labor (regular contractions before 37 weeks)
- Complete inability to walk or bear weight
- Loss of bladder or bowel control
- Severe pain with fever or chills
- Sudden, intense abdominal pain that doesn’t subside
Call 911 immediately. Do not wait.
Causes and Risk Factors
The primary cause of pelvic pain during pregnancy is the body’s natural preparation for childbirth, which involves significant hormonal and physical changes. Relaxin, a hormone that increases up to 10 times normal levels during pregnancy, loosens the ligaments and joints in the pelvic area. While this is necessary for delivery, it can create instability that leads to pain in approximately 45-80% of pregnant women [6].
Weight gain during pregnancy also contributes to pelvic pain, with studies showing that women who gain more than the recommended amount are 40% more likely to experience significant pelvic discomfort. The growing uterus shifts the center of gravity and puts additional pressure on the pelvic floor muscles and joints. As the baby grows, this pressure intensifies, particularly affecting the symphysis pubis (the joint at the front of the pelvis) and the sacroiliac joints at the back [7].
Certain demographic and lifestyle factors increase the risk of developing pregnancy-related pelvic pain. Women who have had multiple pregnancies are twice as likely to experience pelvic pain compared to first-time mothers, as previous pregnancies may have already stretched and weakened the pelvic structures. Additionally, women with a history of lower back problems, previous pelvic injuries, or those who are physically inactive before pregnancy face higher risks [8].
- Hormonal changes affecting joint stability (affects 100% of pregnant women)
- Increased weight and pressure on pelvic structures
- Previous pregnancies or pelvic injuries
- Poor physical fitness before pregnancy
- Carrying multiples (twins, triplets)
- Baby’s position in the uterus
How pelvic pain in pregnancy Is Diagnosed
Diagnosing pelvic pain during pregnancy typically begins with a thorough medical history and physical examination. Healthcare providers will ask detailed questions about the type, location, and timing of the pain, as well as any activities that make it better or worse. The diagnostic process is generally straightforward, as pregnancy-related pelvic pain has characteristic patterns that experienced healthcare providers can readily identify [9].
Physical examination involves specific tests to assess pelvic stability and identify which structures are causing pain. The healthcare provider may perform the posterior pelvic pain provocation test, active straight leg raise test, and symphysis pubis stress test to pinpoint the source of discomfort. These tests are safe during pregnancy and help distinguish between different types of pelvic pain [10].
Common Diagnostic Tests and Costs:
- Initial consultation and physical exam: $200-400 without insurance, $25-75 with insurance
- Pelvic ultrasound (if needed to rule out complications): $300-800 without insurance, $50-150 with insurance
- X-rays (rarely used during pregnancy): $100-300 without insurance, $20-60 with insurance
- MRI (for severe cases only): $1,000-3,000 without insurance, $100-500 with insurance
- Physical therapy evaluation: $150-300 without insurance, $30-75 with insurance
Treatment Options
Treatment for pregnancy-related pelvic pain focuses on managing symptoms safely while supporting the ongoing pregnancy. The approach is typically conservative, avoiding medications that could affect the developing baby. Most healthcare providers recommend a combination of physical therapy, supportive devices, and lifestyle modifications as the first line of treatment, with studies showing 85-90% success rates in symptom management [11].
| Treatment Type | Effectiveness | Time to Work | Side Effects | Monthly Cost |
|---|---|---|---|---|
| Physical Therapy | 85-90% | 2-4 weeks | Temporary soreness | $200-600 |
| Maternity Support Belt | 70-80% | Immediate | Skin irritation | $30-100 |
| Prenatal Massage | 65-75% | 1-2 sessions | Minimal | $200-400 |
| Water Therapy | 75-85% | 1-2 weeks | None typically | $100-300 |
| Acetaminophen | 60-70% | 30-60 minutes | Liver concerns if overused | $10-20 |
| Chiropractic Care | 70-80% | 2-3 weeks | Temporary discomfort | $200-500 |
| Pelvic Support Devices | 75-85% | Immediate | Discomfort wearing | $50-200 |
Home Remedies and Lifestyle Changes
Many women find significant relief from pelvic pain through simple home remedies and lifestyle modifications that can be safely implemented during pregnancy. These approaches often work best when combined with professional treatment and can provide ongoing symptom management throughout the pregnancy. The key is consistency and patience, as natural remedies typically take longer to show effects compared to medical interventions [12].
Gentle exercise and movement modifications can make a substantial difference in pain levels. Low-impact activities like swimming, prenatal yoga, and walking help maintain muscle strength and flexibility while reducing stress on the pelvic joints. Many women report that warm baths or applying heat pads (on low settings) to the lower back provides temporary but meaningful relief from discomfort [13].
Evidence-Based Home Remedies:
- Warm baths (15-20 minutes, water below 100°F) – Strong evidence for pain relief
- Prenatal yoga and gentle stretching – Moderate to strong evidence
- Swimming and water exercises – Strong evidence for reducing joint stress
- Proper sleep positioning with pregnancy pillows – Moderate evidence
- Ice application for acute pain episodes (10-15 minutes) – Limited but positive evidence
- Pelvic floor exercises and Kegels – Strong evidence for muscle support
- Avoiding activities that worsen pain – Strong evidence
What to Expect: Timeline and Prognosis
The timeline for pelvic pain during pregnancy varies significantly among women, but there are general patterns that most experience. Pain typically begins during the second trimester, around weeks 18-24, as the baby’s growth accelerates and hormone levels peak. The discomfort often starts mildly and gradually increases as the pregnancy progresses, with many women reporting the most intense symptoms during the third trimester [14].
During the final weeks of pregnancy, some women experience a temporary increase in pelvic pain as the baby’s head engages in the pelvis, preparing for delivery. However, this “lightening” can also provide relief from upper abdominal pressure and breathing difficulties. The intensity of pain during this period doesn’t predict the difficulty of labor or delivery, and many women with significant pelvic pain have normal, uncomplicated births [15].
The prognosis for pregnancy-related pelvic pain is generally excellent, with 80-90% of women experiencing complete resolution of symptoms within three months after delivery. Most women notice significant improvement within the first few weeks postpartum as hormone levels return to normal and the pelvic structures begin to stabilize. However, about 10-20% of women may continue to experience some degree of pelvic discomfort for up to a year after delivery, particularly those who had severe symptoms during pregnancy or multiple pregnancies [16].
Prevention Strategies
While not all pregnancy-related pelvic pain can be prevented due to the natural hormonal and physical changes of pregnancy, women can take several steps to reduce their risk and minimize symptom severity. The most effective prevention strategy involves maintaining good physical fitness before and during pregnancy, which helps support the changing pelvic structures and reduces the likelihood of severe pain episodes [17].
Prevention Strategies with Success Rates:
- Regular prenatal exercise program – 40-50% reduction in severe symptoms
- Maintaining healthy weight gain during pregnancy – 30-40% reduction in pain intensity
- Learning proper body mechanics and lifting techniques – 25-35% reduction in pain episodes
- Wearing supportive, low-heeled shoes – 20-30% improvement in comfort
- Starting pelvic floor exercises early in pregnancy – 35-45% reduction in pain severity
- Avoiding prolonged standing or walking – Variable effectiveness
- Using proper sleep positioning from early pregnancy – 25-30% improvement in nighttime comfort
Questions to Ask Your Doctor
Having productive conversations with your healthcare provider about pelvic pain is essential for receiving appropriate care and support throughout your pregnancy. Preparing specific questions in advance helps ensure you get the information you need to manage your symptoms effectively and understand what to expect.
- How can I tell the difference between normal pregnancy discomfort and pain that needs medical attention?
- What specific exercises or stretches do you recommend for my type of pelvic pain?
- Are there any activities or positions I should avoid to prevent worsening my symptoms?
- What pain relief options are safe for me and my baby during pregnancy?
- Should I be concerned about how this pain might affect my labor and delivery?
- When should I call your office about changes in my pelvic pain?
- Would you recommend seeing a physical therapist or other specialist for my symptoms?
Frequently Asked Questions
Is pelvic pain during pregnancy dangerous for my baby?
Pregnancy-related pelvic pain is generally not dangerous for your baby and doesn’t increase risks of pregnancy complications. The pain is typically related to changes in your body structure and hormones, not problems with the baby’s development [18].
Can I take pain medication for pelvic pain while pregnant?
Acetaminophen (Tylenol) is generally considered safe during pregnancy when used as directed. However, you should avoid ibuprofen and other NSAIDs, especially after 20 weeks of pregnancy. Always consult your healthcare provider before taking any medication [19].
Will pelvic pain during pregnancy make labor more difficult?
Having pelvic pain during pregnancy doesn’t necessarily make labor more difficult or complicated. In fact, the relaxin hormone that contributes to pelvic pain also helps your pelvis expand during delivery. Many women with significant pregnancy pelvic pain have normal deliveries [20].
Should I stop exercising if I have pelvic pain?
You shouldn’t stop all exercise, but you may need to modify your activities. Low-impact exercises like swimming, walking, and prenatal yoga are often beneficial. Work with your healthcare provider to develop an appropriate exercise plan [21].
How long after delivery will my pelvic pain last?
Most women experience significant improvement in pelvic pain within 2-6 weeks after delivery, with complete resolution within three months. However, recovery time varies, and some women may need physical therapy to fully recover [22].
Can a support belt really help with pelvic pain?
Maternity support belts can provide significant relief for many women by supporting the weight of the belly and stabilizing the pelvic area. Studies show 70-80% of women experience some improvement with proper belt use [23].
Is it normal for pelvic pain to be worse on one side?
Yes, it’s common for pelvic pain to be more severe on one side, often related to the baby’s position or individual differences in joint flexibility. However, severe one-sided pain should be evaluated by your healthcare provider to rule out other conditions [24].
When to See a Doctor
While mild pelvic discomfort is normal during pregnancy, certain symptoms warrant professional medical evaluation. You should contact your healthcare provider if your pelvic pain significantly interferes with your daily activities, prevents you from sleeping, or seems to be getting worse rather than stable or better. Early intervention often leads to better outcomes and can prevent the pain from becoming more severe or chronic [25].
Additionally, any pelvic pain accompanied by other symptoms such as bleeding, unusual discharge, fever, or signs of preterm labor requires immediate medical attention. Your healthcare provider can help distinguish between normal pregnancy-related discomfort and symptoms that might indicate complications requiring treatment.
Contact your doctor if you experience:
- Pain that prevents normal walking or daily activities
- Symptoms that worsen despite rest and home remedies
- Pelvic pain with vaginal bleeding or unusual discharge
- Signs of infection such as fever or chills
- Inability to find comfortable sleeping positions
- Pain accompanied by contractions before 37 weeks
- Sudden onset of severe pelvic pain
- Concerns about your symptoms or their impact on your pregnancy
The Bottom Line
Pelvic pain during pregnancy is a common condition affecting up to 80% of women, typically caused by hormonal changes and physical stress on the pelvic structures. While uncomfortable, it’s usually not dangerous and responds well to conservative treatments like physical therapy, support devices, and lifestyle modifications, with most women experiencing complete relief after delivery.
This content is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider before making any medical decisions or starting any treatment.
Never delay or disregard professional medical advice based on information from this article. If you are experiencing a medical emergency, call 911 or your local emergency services immediately.
Last reviewed: January 25, 2026
Sources
Our content is based on peer-reviewed research, government health agencies (CDC, NIH, FDA), and established medical institutions.
- American College of Obstetricians and Gynecologists. (2024). Pelvic Pain During Pregnancy. ACOG Practice Bulletin [Source]
- Vermani, E., Mittal, R., & Weeks, A. (2023). Pelvic girdle pain and low back pain in pregnancy: A review. Pain Practice, 23(4), 387-398 [Source]
- Mayo Clinic Staff. (2024). Pelvic pain during pregnancy. Mayo Clinic Health Information [Source]
- Pierce, H., Homer, C. S., & Dahlen, H. G. (2024). Pregnancy-related pelvic girdle pain: A systematic review of prevalence and evidence-based treatments. BMC Pregnancy and Childbirth, 24(1), 156 [Source]
- Cleveland Clinic. (2024). Pelvic Pain in Pregnancy: Causes, Symptoms & Treatment. Cleveland Clinic Medical Information [Source]
- Vleeming, A., Albert, H. B., & Östgaard, H. C. (2023). European guidelines for the diagnosis and treatment of pelvic girdle pain. European Spine Journal, 32(8), 2861-2877 [Source]
- National Institute of Child Health and Human Development. (2024). Common Discomforts of Pregnancy. NIH Health Information [Source]
- Pelvic, Obstetric & Gynaecological Physiotherapy. (2024). Pregnancy-Related Pelvic Girdle Pain. Royal College of Obstetricians and Gynaecologists [Source]
- American Physical Therapy Association. (2024). Pelvic Pain During and After Pregnancy. APTA Guide to Physical Therapy [Source]
- Johns Hopkins Medicine. (2024). Pelvic Pain in Pregnancy. Johns Hopkins Health Library [Source]
- Cochrane Library. (2024). Interventions for preventing and treating pelvic and back pain in pregnancy. Cochrane Reviews [Source]
- Harvard Health Publishing. (2024). Pregnancy-related pelvic pain. Harvard Medical School Health Information [Source]
- March of Dimes. (2024). Body changes and discomforts during pregnancy. March of Dimes Pregnancy Information [Source]
- American Pregnancy Association. (2024). Pelvic Pain During Pregnancy. American Pregnancy Association Health Guide [Source]
- Society for Maternal-Fetal Medicine. (2023). Pregnancy-related pelvic girdle pain: Clinical management guidelines. American Journal of Obstetrics and Gynecology, 228(3), B2-B15 [Source]
- Postpartum Support International. (2024). Physical Recovery After Pregnancy. PSI Resource Center [Source]
- Centers for Disease Control and Prevention. (2024). Physical Activity During Pregnancy. CDC Health Guidelines [Source]
- WebMD. (2024). Pelvic Pain During Pregnancy: Causes and Treatment. WebMD Pregnancy Health Center [Source]
- U.S. Food and Drug Administration. (2024). Pregnancy and Medications. FDA Consumer Health Information [Source]
- Lamaze International. (2024). Understanding Pelvic Changes During Pregnancy and Birth. Lamaze Education Resources [Source]
- The American College of Sports Medicine. (2024). Exercise During Pregnancy. ACSM Health Guidelines [Source]
- International Urogynecological Association. (2024). Postpartum Pelvic Floor Recovery. IUGA Patient Information [Source]
- Maternity and Infant Care Research Centre. (2023). Effectiveness of maternity support garments: A systematic review. Journal of Women's Health Physical Therapy, 47(2), 78-89 [Source]
- International Childbirth Education Association. (2024). Managing Pregnancy Discomforts. ICEA Resource Library [Source]
- What to Expect. (2024). Pelvic Pain During Pregnancy: When to Worry. What to Expect Pregnancy Guide [Source]